The most important takeaways when evaluating gastric sleeve vs bypass include:
- How they work: Both make you feel full sooner while eating. Only sleeve makes you feel less hungry generally, and only bypass reduces the amount of minerals your body absorbs.
- Qualify: Each procedure has the same requirements (30+ BMI with health problems, 40+ without)
- Hospital & recovery: Sleeve is a less complicated procedure with a shorter operating time. In-hospital and post-op recovery is similar.
- Weight loss & health improvement: Each procedure is similar at 2 years post-op, but bypass patients tend to keep more weight off over the long-term.
- Insurance: The both have the same coverage (if your policy covers bariatric surgery, both sleeve and bypass will be covered).
- Cost: The both cost the same with insurance, but bypass is about 25% more expensive without insurance.
- Diet & life after: The each have a similar diet and exercise regimen, but bypass requires stricter supplementation and vitamin level monitoring.
- Complications & side effects: Both procedures have a 99.8% survival rate. Bypass has a higher risk of complications and side effects.
Read and click the sections below for everything you need to know to decide which procedure is best for you.
TABLE OF CONTENTS
Click on any of the topics below to jump directly to that section
- How Each Procedure Works
- Weight Loss
- Health Benefits
- Qualify
- Insurance
- Cost Without Insurance
- Recovery
- Diet & Life After
- Downsides
- Summary
- Patient Community & Expert Advice
- Find a Gastric Sleeve or Bypass Surgeon

SECTION SUMMARY:
- The gastric sleeve makes you feel less hungry & feel full sooner while eating. As result you eat less and lose weight.
- If you undergo gastric bypass surgery, you'll feel full sooner while eating & absorb fewer minerals. As a result you'll lose weight.
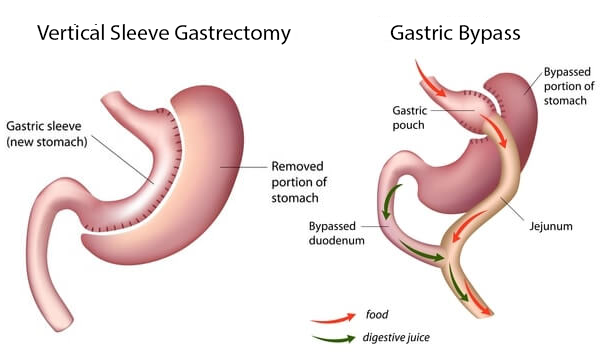
Understanding gastric sleeve surgery vs gastric bypass surgery starts with the fundamental differences in how each alters your anatomy:
Gastric Sleeve
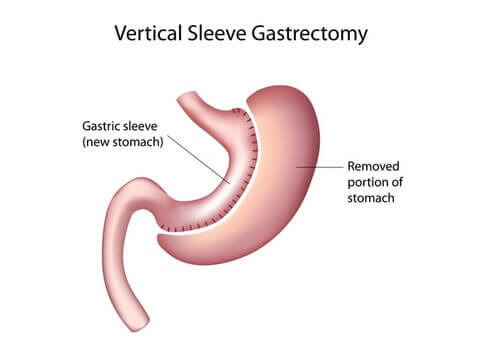
Why Gastric Sleeve Works
- Reduced stomach size makes the patient feel full sooner after eating
- Removed portion of the stomach means fewer hunger-causing hormones are secreted, causing patient to feel less hungry generally
How Gastric Sleeve Is Performed
Gastric sleeve surgery, also called the Vertical Sleeve Gastrectomy (VSG), is performed by removing a large portion of the stomach to create a long pouch that connects the esophagus to the small intestine. The pouch is stapled and the rest of the stomach is removed. Some surgeons take an additional step to reinforce the staple line, although whether that is effective is up for debate.
Gastric Bypass
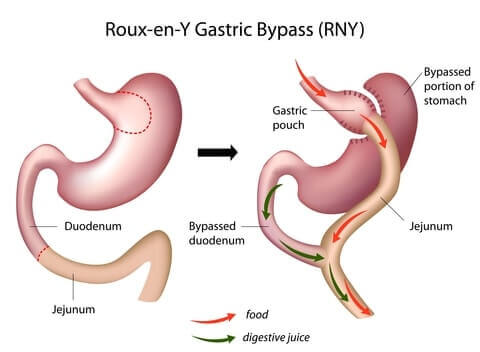
Why Gastric Bypass Works
- Reduced stomach size makes the patient feel full sooner after eating
- Rearranged intestines causes the body to absorb fewer minerals
- Dumping syndrome symptoms deter patients from eating unhealthy foods
How Gastric Bypass Is Performed
Gastric bypass, also called Roux-en-Y gastric bypass or RNY for short, is performed using the following steps:
- Cut and staple the top portion of the stomach to create a small pouch at the end of the esophagus
- Leave the remainder of the stomach attached to the top of the small intestines
- Go further down the small intestine, cut it, and attach it to the pouch
- Take the end of the small intestine that is still connected with the non-pouch portion of the stomach and attach it to the bottom of the “Roux limb.” This allows the digestive juices produced by the stomach to “meet up” with the food in the intestines.
SECTION SUMMARY:
- Gastric sleeve and gastric bypass surgery result in about the same amount of weight loss at the 2-year mark
- Gastric bypass patients tend to regain less weight after the 2-year mark
Patients lose weight quickly after gastric bypass and gastric sleeve, with the low point coming 12 to 18 months after the surgery:
- 3 months: Lose 30% of excess weight
- 6 months: Lose 50% of excess weight
- 1.5 years: Lose 65% to 70% of excess weight
However, bypass patients tend to regain less weight 2+ years after the procedure because:
- The gastric bypass pouch is smaller and therefore less able to stretch out
- Gastric bypass is “mineral malabsorptive” while gastric sleeve is not (body absorbs fewer minerals after gastric bypass)
For more information about gastric sleeve weight loss, see our Project Your Gastric Sleeve Weight Loss page.
For pictures of patients before and after each procedure, including women, men, and celebrities, see the following pages:

SECTION SUMMARY:
- Gastric bypass surgery delivers slightly better overall health improvements
Studies evaluating gastric bypass vs. gastric sleeve have found very similar health improvement for diabetes, hypertension, sleep apnea, and most other obesity-related health problems, depending on which study is referenced.
However, gastric bypass:
- Has a longer list of improved health conditions
- Is more likely to improve most obesity-related health conditions
These surgeries can improve joint health. For every pound of weight lost, there is a 4 pound reduction in pressure on the knee joint (1). This improves mobility and reduces pain in the knees.
Both surgeries were part of research on cancer that included over 88,000 participants. Patients who undergo weight loss surgery have 33% less risk of developing cancer (2).
Risk rates were even further reduced for obesity-related cancers, including (3):
- Colon cancer
- Postmenopausal breast cancer
- Endometrial cancer
- Pancreatic cancer
The chart below compares study results by condition for each procedure:
Tap here to expand a chart that compares health improvement for each procedure.
| Co-morbidity | Gastric Sleeve % Improved /Resolved | Bypass % Improved /Resolved |
|---|---|---|
| Dyslipidemia hypercholesterolemia | 64% | 63% |
| Diabetes | 55% | 83% |
| Hyperlipidemia (high levels of fat in the blood, high cholesterol) | 35% | 73% |
| High Blood Pressure (hypertension) | 68% | 69% |
| Joint/Bone Disease (osteoarthropathy) | 46% | 43% |
| Depression | Most | Most |
| Migraines | 40% | 57% |
| Pseudotumor cerebri | n/a | 96% |
| Cardiovascular Disease | 100% | 79% |
| Venous Stasis Disease | 95% | 95% |
| Gastroesophageal Reflux Disease (GERD) | 50% | 80% |
| Non-Alcoholic Fatty Liver Disease | n/a | 90% |
| Mortality Reduction/ Life Expectancy (5 year mortality) | 89% | 89% |
| Quality of Life Improvements | 93% | 95% |
| Metabolic Syndrome | 62% | 80% |
| Polycystic Ovarian Syndrome | Most | Most |
| Pregnancy | Most | Most |
| Asthma | 90% | 80% |
| Obstructive Sleep Apnea | 62% | 98% |
| Stress Urinary Incontinence | 90% | 88% |
SECTION SUMMARY:
- Gastric Bypass & Gastric Bypass both require a BMI over 40 to "automatically" qualify
- You can also qualify if you have a BMI over 35 if you have severe obesity-related health issues
In order to have gastric bypass surgery or gastric sleeve surgery, your body mass index (BMI) must fall within one of the following ranges:
- Body mass index 40 or above or
- Body mass index from 35 to 40 as long as you have a serious obesity-related health problem (“comorbidity”) such as diabetes, asthma, hypertension, joint problems, sleep apnea, or one of many others.
- Body mass index from 30 to 35 may be accepted if certain health issues are present
For more information on gastric sleeve and gastric bypass qualifications, see the links below:

SECTION SUMMARY:
- Gastric sleeve and gastric bypass are covered by medical insurance, as long as your policy includes bariatric surgery
As long as your specific insurance policy includes weight loss surgery, gastric sleeve surgery and gastric bypass surgery will be covered.
The weight loss surgery insurance approval process can take anywhere from 1 to 12 months, depending on your insurance company and your situation.
Click Here to Check Your InsuranceFollowing are the typical steps:
- Confirm with your doctor that your body mass index and health conditions fall within one of the two qualification requirements:
- BMI over 40 –OR–
- BMI over 35 with one or more of the following (insurance companies will usually not cover BMI’s below 35):
- Clinically significant obstructive sleep apnea
- Coronary heart disease
- Medically refractory hypertension
- Type 2 diabetes mellitus
- Other obesity-related health issues
- Complete 3 to 7 consecutive months of a medically supervised diet program, depending on your insurance company (can be coordinated by your bariatric surgeon).
- Schedule a consultation with your bariatric surgeon.
- Schedule a consultation with your primary care physician to obtain a medical clearance letter.
- Schedule a psychiatric evaluation to obtain a mental health clearance letter (usually coordinated by your bariatric surgeon).
- Schedule a nutritional evaluation from a Registered Dietitian (usually coordinated by your bariatric surgeon).
- Send all of the above documentation to your insurance company along with a detailed history of your obesity-related health problems, difficulties, and treatment attempts. The review process typically happens in under one month (usually coordinated by your bariatric surgeon).
- Insurance company sends approval or denial letter:
- If approved, your surgeon’s bariatric coordinator will contact you for scheduling.
- If denied, you can choose to appeal the denial.
Take the Easy Route – Your surgeon’s office will do most of this legwork for you. They are highly experienced in managing the process and may even have all of the required personnel on staff (e.g. registered dietitian, psychiatrist, bariatric coordinator, etc.).
Click here to find a gastric sleeve or gastric bypass surgeon near you to get started. Most offices will check your insurance for free to confirm coverage criteria.
For more information about weight loss surgery insurance, see our Bariatric Surgery Insurance Guide.
SECTION SUMMARY:
- Gastric sleeve surgery costs about $19,000
- Gastric bypass surgery costs $24,000
The cost of surgery should not dictate which procedure you have. You should move forward with the procedure that is most likely to work for you after thorough research and a consultation with your surgeon.
Still, if you don’t have insurance that covers bariatric surgery, there will be a noticeable difference in gastric bypass vs gastric sleeve cost:
- Gastric sleeve: Average cost is about $19,000
- Gastric bypass: Average cost is about $24,000
Surgeons in your area may charge as low as $10,000 for gastric sleeve or $15,000 for gastric bypass.
Financing may also be available, depending on your credit. Payments are likely to be around the following if your procedure is financed over 5 years:
- Gastric sleeve: $445/mo
- Gastric bypass: $556/mo
Visit our Financing Weight Loss Surgery page for all the possible ways to finance your surgery.
Cost of Not Having Surgery vs. Cost of Weight Loss Surgery
Even if you’re paying out of pocket, the cost of gastric bypass and gastric sleeve is far less than the long-term costs of obesity-related health problems for morbidly obese people who don’t have surgery
On average, weight loss surgery patients pay off their entire surgery and start getting ahead financially after only 2 years (4).
To illustrate: One study found that bariatric patients pay as much as $900 less per month as soon as 13 months after surgery than similar people who didn’t have surgery (5). Starting in month 13, that’s almost $11,000 saved per year in total medical costs.
Fewer prescription drugs alone have been found to save patients $3,000 or more per year (6).

SECTION SUMMARY:
- You'll be "fully recovered" from both in 4 - 6 weeks
Recovery from both gastric sleeve surgery and gastric bypass surgery includes:
- Timeline: 4 to 6 weeks to full recovery
- Hospital Stay: 2 to 3 days
- Time Off Work: 1 to 3 weeks
- Pain: Same as experienced after any laparoscopic surgery, managed with medication
- Diet: Slow transition from clear liquids to solid foods
- Activity: Slow transition back to regular activity and exercise
See the following pages for more information about gastric bypass vs gastric sleeve recovery:
SECTION SUMMARY:
- Gastric bypass and gastric sleeve require very similar dietary changes
- Overall, you’ll feel less hungry after gastric sleeve surgery
- Gastric bypass requires more lifelong vitamin and mineral supplementation
Diet: Gastric Sleeve Vs. Bypass
Your gastric sleeve vs gastric bypass diet transition is virtually identical:
- 2+ Weeks Before – Practice your post-surgery diet
- 2 Weeks Before – High protein, low sugar, low carbs
- 1 Week Before – Stop or change some medications
- 2 Days Before – Clear liquids only
- Midnight Before Surgery – Nothing to eat or drink
- In Hospital to 7 Days After Surgery (Varies by Surgeon) – Sugar-free clear liquids only
- Day 1 to Week 2 After Surgery (Varies by Surgeon) – Add thicker drinks & smooth foods
- Day 2 to Week 3 After Surgery (Varies by Surgeon) – Slowly test pureed foods & soft solid foods
- Day 3 to Weeks 4+ After Surgery (Varies by Surgeon) – Slowly test solid food
The foods you’ll need to avoid are also very similar, although gastric bypass has some additional diet-related aspects to consider.
Diet issues unique to gastric bypass include:
- Avoid foods that are likely to cause dumping, including sugar, unnecessary fat, or refined carbohydrates (although you should avoid these after gastric sleeve as well, they won’t cause dumping for sleeve patients).
- Patients who undergo the bypass procedure are at especially high risk of developing Alcohol Use Disorder (AUD) (7) (8) (9)
Following are dietary guidelines for both gastric bypass and gastric sleeve:
- Test one food at a time to make sure you can tolerate it
- Eat proteins first, in solid form (e.g., not protein shakes)
- Eat healthy “whole” foods
- Avoid processed foods
- Avoid sugary foods or drinks
- Eat slowly and chew thoroughly
- No starchy foods like rice, bread, and pasta
- Avoid any food that is difficult to digest (may be able to tolerate over time), such as:
- Fibrous vegetables like broccoli, celery, and corn
- Nuts
- Seeds
- Skin of any meat
- Tough meats
- Avoid whole milk products
- Drink 64+ oz (2+ liters) of fluids spread throughout the day
- No drinking 30 minutes before or after meals (other than gastric balloon)
- Alcohol only in moderation
See the following pages for more information:
- Bariatric Diet – Compare All procedures
- Gastric Sleeve Diet – All You Need to Know
- Gastric Bypass Diet – All You Need to Know
Vitamins: Gastric Sleeve Vs Bypass
Due to gastric bypass surgery’s higher levels of malabsorption, gastric bypass patients:
- Are much more likely than gastric sleeve patients to require Thiamin (Vitamin B1) supplementation
- Must be more vigilant in confirming no vitamin or mineral deficiencies
The rest of the vitamin requirements are usually the same for gastric bypass and gastric sleeve, including:
- Daily multivitamin
- 1 to 2 per day, forever
- Chewable or liquid versions are best (instead of tablets)
- Take with food (except dairy) to maximize absorption
- At least 200% of the Recommended Dietary Allowance (RDA) of iron, folic acid, thiamine, copper, selenium and zinc
- Daily calcium supplement, in the form of calcium citrate
- Must be calcium citrate (NOT other forms of calcium)
- 1000-1500 mg. daily, forever
- Chewable and liquid versions are best (instead of tablets)
- Try to find one that includes Vitamin D
- Take 2 hours apart from Iron supplements (or Multivitamin that contains Iron) to maximize absorption
For either procedure, you may be required to take one or more of the following depending on your vitamin levels:
- Folate (folic acid)
- Iron
- Thiamin (Vitamin B1)
- Vitamin D
Exercise: Gastric Sleeve Vs Gastric Bypass
After you’ve full recovered from surgery (4 to 6 weeks), recommended exercise is the same for both gastric bypass and gastric sleeve patients: 2.5 hours per week, spread out over 2 to 4 days.
Following this regimen will cause you to:
- Lose more weight
- Be more physically and mentally healthy
Learn more on our Exercise After Weight Loss Surgery page.
Hunger: Gastric Bypass Vs Sleeve
After gastric sleeve, you are likely to feel less hungry as a result of 80% of your stomach being removed. This is not the case after gastric bypass because all of the stomach remains in place (although the stomach will be separated into two parts).
Here’s why gastric sleeve reduces hunger:
When your stomach is empty, it secretes a hormone called ghrelin into your bloodstream which causes your brain to generate hunger impulses. After you eat, the amount of secreted ghrelin drops then slowly rises until your next meal. Since your stomach will be significantly smaller after gastric sleeve surgery, the amount of ghrelin the stomach secretes – and your resulting feelings of hunger – may also go down.
Food Addiction: Gastric Bypass Vs Sleeve
Regardless of which procedure you have, food addiction could be a problem.
Our bodies secrete certain hormones, like ghrelin mentioned above, that tell us when we’re hungry and full, but hyperpalatable food (like junk food) may be overriding those hormone signals by overstimulating our reward centers, much like our bodies and brains react to an addictive drug.
You may have a bona fide food addiction if your desire for food takes priority over other parts of your life that you acknowledge to be more important, such as personal health, family, friends, work, your appearance, or avoiding obesity related health issues like hypertension, sleep apnea, or diabetes.
If left unchecked, food addiction can lead to obesity. For weight loss surgery patients, if not addressed prior to surgery, it can also lead to weight regain.
To find out if you may be suffering from food addiction, take our Food Addiction Quiz.
Relationships After Weight Loss
Significant weight loss after any type of bariatric surgery can lead to big changes with everyone around you.
While many of those changes are positive, some can also be extremely challenging and unexpected.
See our Relationships After Weight Loss Surgery page for important changes to prepare for.

SECTION SUMMARY:
- Gastric sleeve and gastric bypass share most side effects and complications
- Gastric bypass has additional side effects and complications risks (details below)
- Gastric sleeve patients are more likely to regain weight in the future
Gastric sleeve vs bypass challenges are similar, with a few exceptions.
After each procedure:
- Most side effects like nausea, digestive issues, and body changes go away over time or after adjusting diet/lifestyle habits.
- Sagging skin is an issue for some patients, depending how much weight is lost, age, and whether the patient is a smoker
The following challenge is unique to gastric sleeve:
- Weight regain is more likely after sleeve due to the larger sleeve stomach and since it does not include a malabsorptive component
The following challenges are unique to gastric bypass:
- Dumping syndrome is an issue for most patients when they eat the wrong foods. It happens as a result of food (especially sugar) moving too quickly from the stomach into the small intestines and includes symptoms like nausea, diarrhea, bloating, fainting, anxiety, and weakness. It is usually treated effectively by diet changes and/or lying down after eating.
- More likely to develop a vitamin or mineral deficiency, so your surgeon will monitor your vitamin levels more closely and prescribe additional supplements as necessary.
- More likely to experience dental problems due to mineral malabsorption.
Full Gastric Bypass Vs Sleeve Downsides Comparison
Tap here to expand Full Gastric Bypass Vs Sleeve Downsides Comparison.
| Issue | Sleeve | Bypass |
|---|---|---|
| Abdominal Discomfort | — | — |
| Abdominal hernia | Yes | Yes |
| Abscess | Yes | Yes |
| Anemia | — | Yes |
| Band Problems (band erosion, band infection, band intolerance, band leak, band slippage) | — | — |
| Blood Clots | Yes | Yes |
| Body Aches | Yes | Yes |
| Body Feeling Changes | Yes | Yes |
| Bowel Function Changes (diarrhea, constipation, foul-smelling bowel movements and flatulence, difficulty swallowing, gurgling noises) | 1Yes | Yes |
| Bowel Obstruction | Yes | About 3% of patients |
| Deep Vein Thrombosis | Yes | Yes |
| Dehydration | Yes | Yes |
| Dental Problems | — | Yes |
| Dumping Syndrome | — | About 70% of patients |
| Dyspepsia (Indigestion) | Yes | Yes |
| Esophageal Dilation | Yes | Yes |
| Esophagitis | Yes | Yes |
| Evisceration & Incisional Hernia | Yes | Yes |
| Food Trapping | — | Up to 2% of patients |
| Gallstones | Up to 1/3 of bariatric patients | Up to 1/3 of bariatric patients |
| Gastric Fistula | Yes | Yes |
| Gastritis | Yes | Yes |
| Gastroesophageal Reflux Disease (GERD) | About 20% after 1 year; About 3% after three years | Yes |
| Gastrointestinal Leaks | About 2% of patients | About 2% of patients |
| General Anesthesia Complications | Yes | Yes |
| Hair Loss | Yes | Yes |
| Heart Attack | Yes | Yes |
| Hemorrhage (Bleeding) | About 1% of patients | About 2% of patients |
| Hiatal Hernia | Yes | Yes |
| Hypoglycemia | — | Yes |
| Infection | Yes | About 3% of patients |
| Intolerance to Certain Foods | Yes | Yes |
| Kidney Stones | — | Yes |
| Marginal Ulcers | Yes | Yes |
| Nausea, Vomiting and/or Stomach Cramps | Yes | Up to 70% of patients |
| Organ Injury During Surgery | Yes | Yes |
| Peritonitis | Yes | Yes |
| Pneumonia | Yes | Yes |
| Port Problems (port flip/ inversion or dislodgement, port leak, port infection, port dislocation) | — | — |
| Pouch Dilation | — | — |
| Pulmonary Embolism | Yes | Yes |
| Respiratory Failure | Yes | Yes |
| Skin Changes (e.g. acne, dry skin, sagging skin, etc.) | Yes | Yes |
| Stenosis/Stricture | About 1% of patients | About 5% of patients |
| Stoma Obstruction | — | — |
| Stroke | Yes | Yes |
| Thrombophlebitis | Yes | Yes |
| Thrush (Yeast Infection) | Yes | Yes |
| Vitamin & Mineral Deficiency / Malnutrition / Malabsorption | Yes | Yes |
| Weight Regain | Yes | Yes |
| Wound Reopening | Yes | Yes |
| Wound Sepsis | Yes | Yes |
For definitions of any issue in the chart, see our Bariatric Surgery Complications page.
SECTION SUMMARY:
- See the "winner" and "loser" by category below
Your individual situation will determine whether gastric bypass or gastric sleeve surgery is best for you. Following is a review of which procedure is “better” in each category discussed on this page.
- Most Popular Procedure: Gastric Sleeve
- Most Short-Term Weight Loss: Tie
- Most Long-Term Weight Loss: Gastric Bypass
- Best Health Improvement Gastric Bypass
- Easiest to Qualify: Tie
- Low-Cost Procedure (With Insurance): Tie
- Low-Cost Procedure (Without Insurance): Gastric Sleeve
- Best Post-Op Diet: Gastric Sleeve
- Fewest Risks & Side Effects: Gastric Sleeve
Discuss each of the pros and cons with your surgeon before making a final decision. Click here to find a weight loss surgeon.

SECTION SUMMARY:
- You can read about the experiences of other gastric sleeve patients
- You Can "Ask the Expert"
If you still have questions about gastric sleeve vs gastric bypass, our experts are happy to answer them. We (and other patients) would also love to hear about your experiences.
Please use the form below to share your experience or ask a question.
Questions From Other Visitors*
Click below to see contributions from other visitors to this page.
Hi, I’m 33 and want weight loss surgery and I’m about 80 pounds overweight. I either want gastric sleeve or gastric bypass. My concern is I have irritable bowel syndrome…
Gastric Bypass Surgery and Smokers*[Review_by_text]Hi everyone, I am scheduled to have my surgery in only a few more weeks and am just planning to begin my pre op phase in a few days. One…
SECTION SUMMARY:
- You can ask a local bariatric practice for a free insurance check or cost quote
- You can attend a free in-person seminar or an online webinar offered by a local weight loss surgeon
- You should schedule a phone or in-person consultation (both often free), if you are interested in learning more about weight loss surgery



