Lap-Band problems:
- Are almost never life-threatening (gastric band surgery has a survival rate of 99.9%)
- Include inadequate weight loss and potential complications
- May or may not require removal of the band
Read the sections below for everything you need to know about adjustable gastric band problems and complications.
TABLE OF CONTENTS
Click on any of the topics below to jump directly to that section

SECTION SUMMARY:
- Lap-Band removal is required in fewer than 1 out of 10 patients
At around 0.1%, LAP-BAND® surgery has an extremely low mortality rate (death rate).
And fortunately, many of the complications are minor and are easily repaired, and the typical worst case is the removal of the band.
At 5 years post-op, LAP-BAND® removal is required in about 9% of patients (fewer than 1 out of 10) who maintain continued interaction with their surgical team and follow established guidelines closely (1).
Studies for Lap Band Problems & Complications
Following are the gastric banding mortality and complication rates from 5 separate studies for patients who did NOT necessarily maintain continued interaction with their surgical team and follow established guidelines closely.
Tap here to expand a table of studies for lap band problems & complications
| Studies | # of gastric banding patients in study | Mortality & Complication Rates | Year |
|---|---|---|---|
| Study F | 714 | Mortality – 0% Revisional procedure required – 50.4% (proximal enlargement (pouch dilation) -26%; band erosion-3.4%; port and tubing problems-21%). STUDY NOTE: “The need for revision decreased as the technique evolved, with 40% revision rate for proximal gastric enlargements in the first 10 years, reducing to 6.4% in the past 5 years. The revision group showed a similar weight loss to the overall group beyond 10 years.” | 2012 |
| Study A | 1,176 | Mortality – 0.09% Major complications – 1% All complications – 2.6% | 2008 |
| Study B | 400 | Mortality -0.25% All complications – 8.8% | 2007 |
| Study C | 179 | Mortality -0.56% Early complications – 2.8% Late complications – 26% 4 Years – 82.1% | 2007 |
| Study E | 190 | Mortality – 0% All complications – 10.5% | 2004 |
SECTION SUMMARY:
- Failure is considered not losing enough weight and/or suffering from a complication that required removing your Lap-Band
There are 2 lap band problems that cause the surgery to be classified as a failure:
- Unsuccessful weight loss – “unsuccessful” carries a different definition with each surgeon, but in general a procedure is considered to be a failure if you lose 25 to 30% or less of your excess weight (in other words, if you’re 100 pounds overweight that would mean you lost 25 to 30 pounds or less).
- Complication(s) requiring the removal of the band.
Our LAP-BAND® Surgery Failure page will take you through the details.

READ THIS FIRST
Are you experiencing complications with your gastric band?
We highly recommend contacting your previous surgeon or a top LAP-BAND® revision surgeon to discuss the issues as soon as possible.
If you have not yet had weight loss surgery and are concerned about potential LAP-BAND® issues, remember that most surgeons offer free seminars and/or free one-on-one consultations that teach you about your options and their office’s specific results, which may vary widely from practice to practice.
Following is a complete list of potential LAP-BAND® problems. We have also included the percentage of patients who experience each when the information is available (where you see a range of percentages, multiple studies were found with varying results) (2) (3) (4) (5) (6) (7) (8).
Click one of the following to jump down to more information or scroll down the page to review the complete list…Real-World Patient Experiences
It’s one thing to read about the potential list and general risks of complications, but it’s quite another to hear first hand how they can affect your life.
- Alcohol Use Disorder (AUD) (11% of gastric banding patients) – a physical and emotional dependence on alcohol that leads to the inability to cease drinking, even after serious lifestyle, health, or legal issues.
- Band problems (1.1% – 18% of gastric banding patients)
- Band erosion (2.1% – 9.5%) – (also called “band migration”) occurs when the band actually grows into the stomach. The only treatment is permanent removal of the band. See our LAP-BAND® Erosion page for more information.
- Band intolerance – some patients’ bodies just can’t handle the band. After all, the band is a foreign object in your body. Band intolerance includes vomiting excessively or feeling uncomfortable all of the time. Permanent removal of the band is required in these cases.
- Band leak (1.1% – 4.9%) – patients can usually tell if their gastric banding system has a leak if their feelings of restriction decrease over time (thus increasing hunger) without the doctor unfilling the port. To determine whether you have a leak, your doctor may inject colored fluid and take an X-Ray to see if any of the colored fluid is present (from a leak) outside of the gastric banding system. Surgery is usually required to repair it.
- Band slippage (2% – 18%) – occurs when the lower part of the stomach “slips” through the band, creating a bigger pouch above the band. Either removing fluid (from the LAP-BAND®) or surgical repositioning is required to repair band slippage. Symptoms include vomiting and reflux, and it is diagnosed by drinking a dye and using X-Ray to observe it. The band placement technique used by the surgeon also makes a difference – between the perigastric technique (PGT) and the pars flaccida technique (PFT), the pars flaccida technique appears to have a much lower rate of slippage (up to 16% less often) (8) (9) (10).
- Blood Clots (also called “thrombus”) – overweight people have a higher risk of developing blood clots during and after any kind of surgery. Blood thinners are often used to help prevent blood clots, along with special devices that squeeze the lower legs (“pneumatic compression devices”) to keep the blood flowing. Walking around periodically after surgery is also very effective. Symptoms of blood clots include swelling or pain in the legs and can be diagnosed by your doctor with an ultrasound. Blood clots are treated by a taking a prescribed blood thinner. If left untreated, clots can lead to a pulmonary embolism. Be sure to tell your doctor whether you or anyone in your family has a history of clotting. Smoking will increase your risk, so if you are a smoker it is recommended that you stop smoking as soon as possible before surgery – no later than two months out. For more information, see our Blood Clot Symptoms, Treatments & Prevention page.
- Bowel Function Changes – bowel function after LAP-BAND® surgery may change, including…
- Constipation– usually corrected by increasing the amount of water you are drinking and by taking fiber supplements such as Fiber-Stat’s liquid fiber supplement.
- Difficulty swallowing (also called “dysphagia”) – caused by eating too quickly, too much or not chewing food enough and can usually be fixed by avoiding these habits.
- Bowel perforations (0.5% – 3.1%) occur when the bowel is punctured during surgery. Perforations are often caught and repaired right away, but it may take hours or days for them to show up, after which surgical repair will be required.
- Esophageal dilation (14%) ("dilated esophagus") is the enlarging of the esophagus and is usually the result of the band being too tight or being placed incorrectly. Most cases can be handled through deflation of the band
under radiological control. GERD symptoms and vomiting are more frequent in patients who develop esophageal dilation.
Also see Achalasia.
- Food trapping occurs when food gets caught in one of the small openings in your digestive system. Food trapping is seen in 1 to 2% of gastric banding patients and is treated by deflating the band entirely until the food passes through.
- Gallstones – small stones of cholesterol formed in the gall bladder or bile passages. Gallstones can be created following rapid weight loss which leads to their development in as many as 1/3 of bariatric surgery patients. As a result, your surgeon may remove your gallbladder during surgery or prescribe bile salt supplements after surgery.
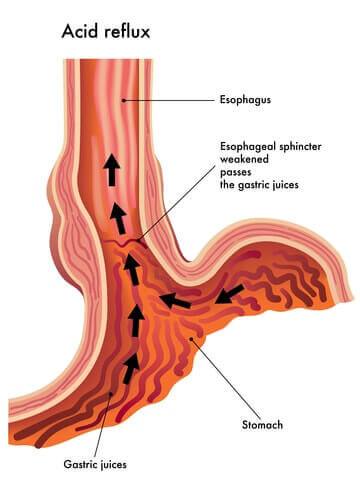
- Gastro-esophageal reflux disease (GERD) – a highly variable chronic condition that is characterized by periodic episodes of gastro-esophageal reflux usually accompanied by heartburn and that may result in histopathologic changes
(change in the microscopic structure) of the esophagus. GERD often leads to esophagitis. While
bariatric surgery can cause GERD, the condition is also improved for many following bariatric surgery.
Several at-home treatments are effective, including avoiding certain foods and drinks (alcohol, citrus juice, tomato-based food and chocolate), waiting 3 hours before lying down after a meal, eating smaller meals and elevating your head 8 inches when you lay down. If these don’t work, your doctor may recommend/prescribe antacids to be taken after meals and before going to bed, H2 blockers or even Proton Pump Inhibitors (PPI).
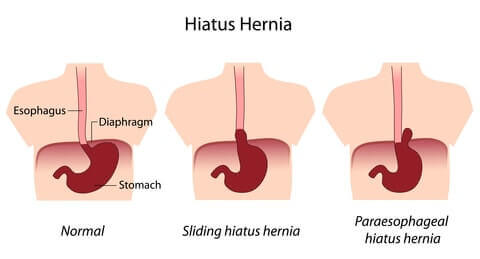
- Hiatal Hernia – a hernia in which an anatomical part (such as the stomach) protrudes through the esophageal hiatus (opening) of the diaphragm. Hiatal hernias can occur after restrictive procedures when food causes the smaller stomach to bulge and push through the diaphragm. It is not uncommon for an obese patient to already have a hiatal hernia before surgery. While a hiatal hernia can be a “contraindication” for surgery (reason that you may not be able to have the surgery), hiatal hernias can also be repaired during bariatric surgery.
- Indigestion (also called “dyspepsia”) – inability to digest or difficulty in digesting food; incomplete or imperfect digestion of food; a case or attack of indigestion marked especially by a burning sensation or discomfort in the upper abdomen. Treatment is usually as simple as changing your diet, such as avoiding greasy foods or only drinking liquids for a certain period of time. Alcohol, aspirin and other drugs are also causes. If diet changes don’t work, antacids and H2 blockers are sometimes prescribed.
- Intolerance to certain foods – With a changed stomach size or digestive system, there will be certain foods that you’ll need to avoid and certain diet habits you’ll need to maintain. See our Bariatric Diet section and Bariatric Eating page (how you eat vs what you eat) for more.
- Nausea and vomiting is one of the most common side effects of bariatric surgery and is experienced in up to 70% of patients. In one study, patients on average reported feeling nauseous 1.4 times per week and vomiting about once per week after gastric banding. Following the doctor’s orders regarding your bariatric diet will typically fix or improve the problem. While in the hospital, receiving a larger amount of IV fluids at a faster rate may make you less likely to feel nauseous or vomit.
- Pneumonia – a disease of the lungs that is characterized especially by inflammation and consolidation of lung tissue followed by resolution, is accompanied by fever, chills, cough, and difficulty in breathing, and is caused chiefly by infection. Obese patients are more likely to develop pneumonia post-surgery, so it is important that patients begin deep breathing and coughing exercises to prevent it. These exercises are much easier after laparoscopic surgery than after open surgery. Should pneumonia develop, it can be treated with antibiotics.
- Port problems (20.5% or about 1 in 5 gastric banding patients), including…
- Port flip/inversion or dislodgement (10.3%) occurs when the LAP-BAND® port (where fluids are taken out or added to the band) “flips over”. This is typically not a serious problem and a quick procedure can turn it back over.
- Port Leak (1.1% – 4.9%) – as with a band leak, patients can usually tell if their gastric banding system has a leak if their feelings of restriction decreases over time (thus increasing hunger) without the doctor unfilling the port. To determine if you have a leak, your doctor may inject colored fluid and take an X-Ray to see if any of the colored fluid is present (from a leak) outside of the gastric banding system. Surgery is usually required to repair it.
- Port or band infection (1.5% – 5.3%) – if port or band infection occurs, it is usually healed with antibiotics, but removal of the band or port may be necessary.
- Port dislocation (6.9%) – similar to a port flip, a port dislocation means that your port has moved from its original location. It can be fixed with a simple operation under local anesthesia.
- Pouch dilation (6.3% – 16.9%) refers to the enlarging of the stomach pouch above the band. It may be fixed by removing fluid from the band, but surgery is sometimes required. Good outcomes can be expected after rebanding in properly assessed patients with slippage and pouch dilation.
See our Bariatric Surgery Complications page for a procedure by procedure comparison of complications along with what you need to do to minimize your risks. Our LAP-BAND® vs Gastric Bypass page provides a more specific comparison between the two most popular bariatric surgery procedures.
Health Risks of Obesity Vs. Risks of Weight Loss Surgery
When deciding whether the risks of complications and mortality are “worth it”, it is a good idea to evaluate the risks of not having surgery. See our Life after Weight Loss Surgery or Obesity Health Problems pages for more on this.
SECTION SUMMARY:
- You can read about the experiences of other gastric sleeve patients
- You Can "Ask the Expert"
Ask the Expert & Patient Experiences*
We would love to hear your experiences with LAP-BAND® problems and complications. Your insights are invaluable to making sure other people have the tools to meet their goals.
We would also be happy to answer any questions you may have about LAP-BAND® problems and complications.
Please use the form below to share your experience or ask a question.
Questions From Other Visitors*
Click below to see contributions from other visitors to this page.
Why do I have so much gas 8 month after lap band surgery? Any help would be greatly appreciated!
Vomiting after lap band fill*I had a fill about three weeks after lap band surgery. Now, in week four, I am starting to vomit everything I eat - even water. Why is this happening…
Can't get a perfect lap band adjustment*I had my lap band surgery in Jan. 2011 and have lost 32 pounds, but I can't seem to get a good adjustment. To my frustration, it took me 5…
No Weight Loss After Lap Band Surgery*On march 15th, 2011 I had my lap band surgery... that was the biggest mistake I made. I fully regret it and now I fell into such a bad depression.I…
Same Amount of Food Regardless of Lap Band Fill Amount*I am female that had my lap band surgery in 2008 and I was 40 years old. My maximum weight was ~245 pounds and I am 5'3". It took two…
Options for Lap Band Slip*I had my lap band procedure three years ago, lost 90 pounds and loved the whole experience. Gradually over the past year I started having GERD-like symptoms to the point…
Lap Band Slippage Symptoms*What are the specific lap band slippage symptoms? It's been seven days since my surgery and I feel like I have slippage. If I put my hand on my stomach,…
Still Vomiting 5 Years After Lap Band*I had a Lap-Band inserted in 2008 and lost 30kg. I learned the hard way which foods I could and couldn't eat. My kids' friends thought I was bulimic. I…
Lap Band Port and Band Not Connected*I had a band put in 2 years ago and was successful - I lost 250 pounds. Last August I went for a routine fill. I was unable to hold…
Enlarged Pouch and Distal Migration of Lap Band*I had the lap band in 2005. My last band fill was in 2006. About six months ago I stared having reflux. My family doctor sent me for EGD it…
Burping Followed by Metal or Blood Taste 5 Years After Lap Band Surgery*I had the lap band surgery about 5-6 years ago and have had several adjustments. Have not had really any problems from my surgery, if I eat too fast and…
Servere burning and pain when I eat and drink 7 years after lap band surgery*It started yesterday, and I thought it was because I ate an orange on an empty stomach and have not eaten one for a year. It felt like the inside…
Ever Heard of Lap Band Port Coming Through Stomach Wall?*My husband and I both have a lap band. He has had a red inflamed area over his port for a few months now. He asked the fill nurse about…
Bad Acid Reflux 1.5 Years After Lap Band Surgery*I have developed bad acid reflux one and a half years after lap band surgery. The reflux is especially bad at night. I have hiccups... from the stomach clear up…
Frequent Vomiting One Year After Lap Band Surgery*My mother had gastric band surgery last year and has been on the new diet since then. But about six months ago she went to the surgeon because she had…
Heartburn After Lap Band Surgery*I had lap band surgery 5 yrs ago. I haven't had heartburn since then until about 2 months ago. I have not changed the way I eat or anything. I…
Port Incision Won't Close After Lap Band Surgery*On July 12th I went in for lap band surgery. My weight on surgery day was 292 pounds. The doctor made 5 entry points on my stomach (the port is…
Vomit 3 to 4 times per day 1.5 years after gastric banding*I had stomach banding surgery on 3/06/2010 and every thing was fine. I began to lose weight immediately and continued to lose until April of 2011 when the vomiting episodes…
Cramp where port is and feeling full of gas*I had my lap band in San Diego (Dr. Bhoyrul) in 2010. I have recently been feeling a contraction of the muscle or stomach where my band is. I have…
My body rejected the band - warning for autoimmune disease patients*This is long but maybe can help enlighten someone. I had a band placed in 2002 after several years of being obese (50-90 lbs overweight) and diets failing me. I…
Pressure & Swelling in Upper Abdomen 3 Years After Lap Band Surgery*Had lap band surgery in 2009 and have started to regain weight in the past year. I've also been having a lot of pressure and swelling in the upper stomach…
Spasms & Fainting Spells After Lap Band Surgery*I had revision surgery over a year ago for slippage of my band. A month after that surgery I started having fainting spells and spasms that originated in my stomach…
Is A Lap Band Revision A Good Idea After Weight Gain?*Hi y'all, I am three years after my Lap-band surgery. My long-term goal was to lose about 50% of my excess weight, which at the time was about 95 pounds.…




